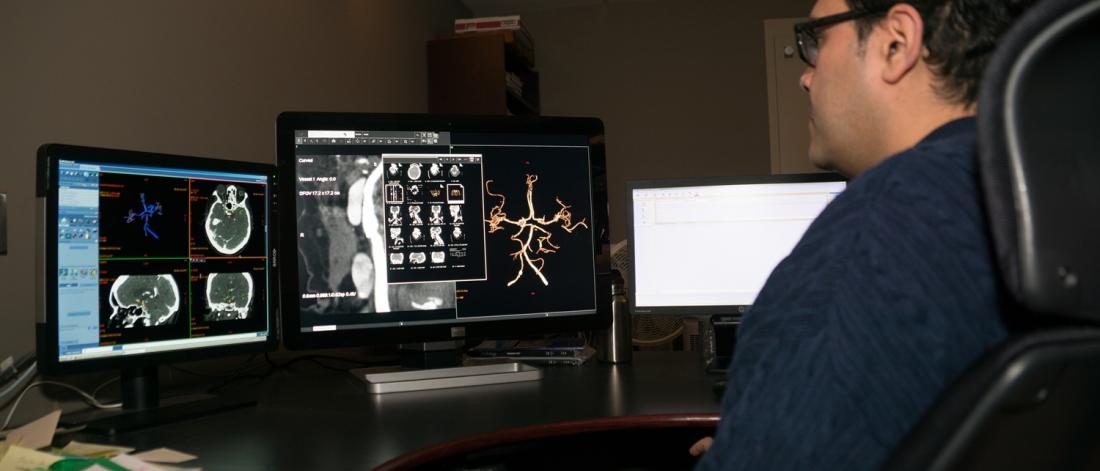
State-of-the-art facilities and equipment
The Health Sciences Centre and Winnipeg Children’s Hospital are equipped with modern diagnostic equipment such as 1.5 and 3T MR imaging (including an intraoperative MRI Suite or IMRIS), high-resolution CT scanning and angiographic capabilities. In addition, the Health Sciences Centre is home to Canada's first Gamma Knife Unit which treats such conditions as metastatic tumours and vascular malformations and attracts clinical research.
Single-site neurosurgery centre
The only referral centre for the 1.2 million Manitoba residents, Winnipeg's Health Sciences Centre, which includes General Hospital and Children's Hospital, has developed uniform protocols for the treatment and long-term follow-up of patients with various neurosurgical disorders.
Program details
Complete residency details, including program curriculum, application requirements and selection criteria can be found on the Canadian Resident Matching Service website.
How to apply for residencies
-
-
To be considered for admission to any residency at the University of Manitoba, you must apply through the Canadian Resident Matching Service (CaRMS).
CaRMS is a national, independent, not-for-profit, fee-for-service organization that provides a fair, objective and transparent application and matching service for medical training throughout Canada.
Explore the University of Manitoba
We attract people from around the world who share our ideals and vision for positive change. We believe in embracing challenges and taking action. Our students, researchers and alumni bring their unique voices to learning and discovery, shaping new ways of doing things and contributing to important conversations in topics that matter most, from human rights to global health to climate change. We are where imagination and action collide.
Contact us
-
Colin Kazina
Program director
Phone: 204-787-8044 -
Program administrator
neurosurg@umanitoba.ca -
Tora Young
Program administrator
Phone: 204-787-8044
Surgery
Max Rady College of Medicine
AE101-820 Sherbrook Street
University of Manitoba (Bannatyne campus)
Winnipeg, MB R3A 1R9 Canada