Reproductive infectious disease
As Canada grapples with a resurgence of syphilis and consequently of congenital disease, Reproductive Infectious Disease (RID) was already providing important leadership in Manitoba. With the onset of the COVID-19 pandemic, innovative care strategies and vision were required to guide rapidly changing needs in obstetrical care. RID subspecialist Dr. Vanessa Poliquin is a Manitoba trailblazer who received the 2020 CMA Award for Young Leaders (Early Career) in recognition of her exemplary dedication, commitment and leadership in clinical, educational and community service. A full compliment of online resources were developed at the department level as well as Provincial Policy for COVID-19 and Women's Health.
Northern remote exposures
Many of Manitoba's rural communities are fly-in only where health needs are supported by small nursing stations. Generalist ObGyns and Gyne Oncologists provide in-community care with monthly or bimonthly visits to a wide catchment of communities from as far north as Rankin Inlet to small island reserves like Little Grand Rapids. Residents all get protected time to participate in these outreach opportunities, but can elect to increase those endeavours to support a passion for Indigenous partnership and advocacy. Dr. Sarah Kean provides oncology access to our patients in the far north, including counselling regarding genetic conditions such as BRCA. Scheduling is overseen by the PGME Program coordinator and travel is in partnership with Ongomiizwin Health Services.
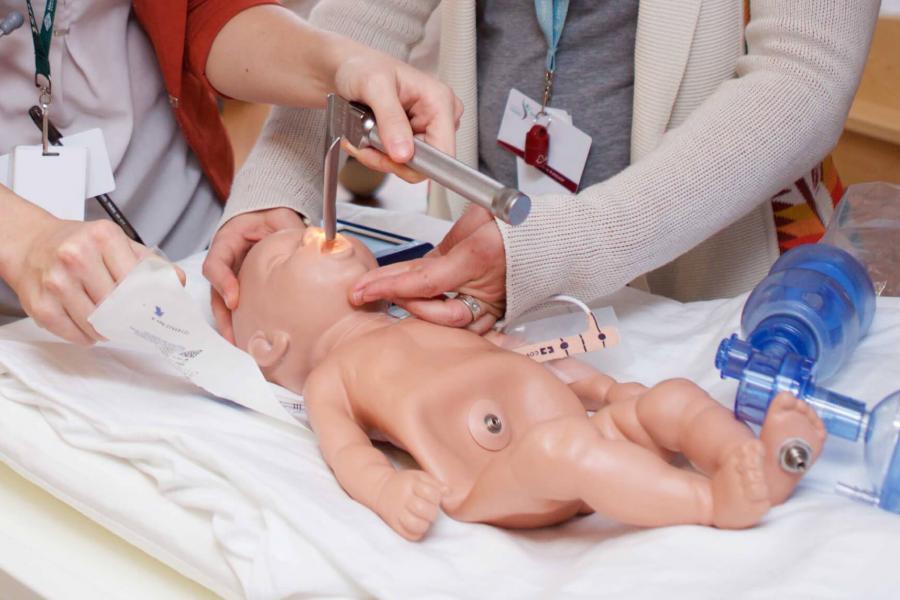
Pediatric obstetrics and gynecology
The unique needs of children and adolescents range from structural anomalies to teen pregnancy and menstrual disorders. This subspecialty features surgical exposures not seen in other areas of obstetrics and gynecology, pubertal changes and disorders such as precocious or delayed development, and the complexities of adolescence in the setting of pregnancy. This program is uniquely partnered with pediatric surgery and provides multidisciplinary care to its young patients. Residents rotate through this program which is rich with research opportunity.
Learners interested in additional exposures or study can contact assistant professor Amanda Morris.
Family planning
Ensuring reproductive choice, be it comprehensive access to contraception or termination services requires advocacy, innovation and vision. Fellowship trained Dr. Helen Pymar developed and continues to oversee the Early Pregnancy Assessment Clinic which offers management of symptomatic first trimester pregnancy to over 1,000 patients each year and is the home to the largest database in Manitoba of ectopic, molar and complicated early pregnancy. Dr. Pymar is winner of multiple teaching awards from UGME and PGME but also keeps her colleagues current with novel treatments like Nexplanon implants and new emergency contraception.
Psychosocial obstetrics
Pregnancy complicated by substance use, homelessness, mental illness and trauma have an excessive burden of morbidity and mortality. Dr. Adelicia Yu has partnered with midwifery colleagues to provide inner-city obstetrical care to the street entrenched population and provided Directorship to the first Psychosocial Obstetrics and Gynecology Fellowship in Canada. Cultivating interprofessional relationships in the community not only provides wrap-around care but enriches innovation opportunity.
What we offer
Excellence in teaching and learning is the driving force behind our academic mission. Our department strives to facilitate a high-quality clinical learning experience for undergraduate students, residents and fellows within our two tertiary care hospitals, as well as a variety of public and private hospitals within Winnipeg.
Our story
Watch a brief video to learn more about our department and what we offer.
Sections within our department
Minimally Invasive Gynecologic Surgery
Gynecologists trained in minimally invasive gynecologic surgery specialize in evaluating and treating people who have a wide range of noncancerous (benign) gynecologic conditions, including heavy menstrual periods (menorrhagia), irregular menstrual periods (metrorrhagia), pelvic pain, endometriosis and ovarian cysts.
Section head: Devon Evans
Section members
Section 2
ewr
Section 3
r
Section 4
f
Awards and scholarships
The Department of Obstetrics, Gynecology and Reproductive Sciences offers several awards based on academic merit and professional achievement.
Dr. A.A. Earn Memorial Award
An endowment fund of $12,300 was established in honour of Dr. A.A. Earn by his wife Josephine, daughter Dinah, and son David. Dr. Earn was a distinguished member of the Department of Obstetrics, Gynecology and Reproductive Sciences from 1959-1995. The award, to be used for the purchase of texts, is valued at $500 and will be awarded annually to a student who:
- is enrolled in the Post Graduate Medical Education program in Obstetrics and Gynecology in the Faculty of Medicine at the University of Manitoba;
- shows exceptional promise in Obstetrics and Gynecology.
Dr. I.C. and Mrs. M. Peever Memorial Fund
A trust fund has been established at the University of Manitoba in memory of Dr. Irvin Carr Peever and Mrs. Muriel Peever. The available annual interest from the fund will be used to offer a prize to a student who:
- is enrolled full-time in the third or fourth year of study in the Postgraduate Medical Education Program (PGME), in the Faculty of Medicine;
- has demonstrated exceptional promise in Obstetrics and Gynecology based on clinical competency and as determined by the selection committee.
Dr. Max Rady Memorial Prize
A bequest of $5,000 has been left to The University of Manitoba by the late Dr. Max Rady to establish an award in the field of Obstetrics and Gynaecology. The award shall be known as the Dr. Max Rady Memorial Prize in Obstetrics and Gynaecology. The value of the prize shall be the annual income of the fund. The prize shall be awarded annually to the best first year resident in Obstetrics and Gynaecology.
Dr. Marvin Raynes Memorial Prize
An award to be called the Dr. Marvin Raynes Memorial Prize, established on behalf of his mother, Mrs. Margaret Raynes, and his sisters, Mrs. Sylvia Berkson and Mrs. Estelle Einsenberg, is available at The University of Manitoba.
This prize shall be awarded annually to a postgraduate resident of exceptional promise in Obstetrics and Gynaecology. The prize shall have an annual value of $100. If further donations to, and earnings of, the fund sustaining the prize permit, the value of the annual award will be increased.
Dr. Michael Bruser Memorial Award
A fund has been established at The University of Manitoba in memory of Dr. Michael Bruser by his colleagues and friends. From the fund an annual award will be made to a second or third year resident in Obstetrics, Gynaecology and Reproductive Sciences division of the Faculty of Medicine.
Whenever possible, preference will be given to residents working in the areas of fetal physiology and fetal heart monitoring, both areas of special interest to Dr. Bruser. The value of the award will be $600. If earnings on, or further contributions to, the fund supporting this award permit, the value of the award will be increased.
Dr. T.J. Lamont Memorial Prize in Maternal and Neonatal Welfare
The Dr. T.J. Lamont Memorial Prize in Maternal and Neo-Natal Welfare was established by Dr. J. Laurie Lamont (B.A. University of Manitoba, M.B.Ch.B. University of Edinburgh) with a donation of $3,000 of Canada Victory Bonds in 1944, to the University of Manitoba. The Prize is a memorial to his father, Dr. T.J. Lamont (1858-1920), a Manitoba Medical College graduate (1889) and a pioneer general practitioner in Treherne, Manitoba, from 1890 to 1920. The purpose of the
Prize is to stimulate interest and research in the area of maternal, peri-natal and neo-natal welfare.
The available annual interest from the fund will be used to offer one prize to a student who:
- is enrolled full-time in the Postgraduate Medical Education Program, up to and including the PGY7 level;
- has presented the best oral or poster presentation of an original work of investigation in maternal, peri-natal, and neo-natal welfare.
In any given year that presentations are judged by the selection committee to be of insufficient merit, the prize will not be offered and the unexpended money will be added to the capital. The selection committee will be named by the Dean of the Faculty of Medicine (or designate) and will include the Heads of the Departments of Community Health Sciences; Obstetrics, Gynecology and Reproductive Health; and Pediatrics (or designates).
The Board of Governors of The University of Manitoba has the right to modify the terms of this award if, because of changed conditions, it becomes necessary to do so. Such modification shall conform as closely as possible to the expressed intention of the donor in establishing the Prize.
Deadline: April 9, 2021
department Research
Research education is an integral goal of the Department of Obstetrics, Gynecology and Reproductive Sciences. Our research is multidisciplinary, collaborating with other faculties such as nursing, anesthesiology, pediatrics, genetic and community health.
We are grateful for the support of local and national funds, including the Manitoba Institute for Child Health, University of Manitoba Research Council, Manitoba Health and the Canadian Institute for Child Health (CIHR).
Our researchers
- Alon Altman
- Alicia Berard
- Adam Burgener
- Margaret Burnett
- Devon Evans
- Jennifer Hunt
- Xiao Qing Liu
- Mark Nachtigal
- Vanessa Poliquin
- Christy Pylypjuk
- Helen Pymar
Research day
Overview
We are pleased to announce the 2024 Department Research Day will be a full-day virtual event that will include presentations from trainees and faculty.
2024 Research Day
Friday, May 10, 2024
Full day | Virtual
Research Day Objectives
At the end of Department Research Day, participants will be able to:
- Understand research methodology, analysis and presentation in obstetrics, gynecology and reproductive sciences
- Identify emerging research within the department and its relationship to clinical practice and future research opportunities to fulfill Royal College training requirement
Accreditation
This event is an Accredited Group Learning Activity (Section 1) as defined by the Maintenance of Certification Program of The Royal College of Physicians and Surgeons of Canada, and approved by the CPD Medicine Program, University of Manitoba for a maximum of 6.0 hours.
Participants should only claim credit for the actual number of hours attended.
The University of Manitoba CPD Medicine Program is fully accredited by the Committee on Accreditation of Continuing Medical Education (CACME).
Registration information
This annual department event will cover a range of topics related to obstetrics and gynecology and provides an opportunity to showcase both project proposals and completed department research.
2024 Research Day
Friday, May 10, 2024
Full day | Virtual
Or scan the QR code below to register.

Event program
Friday, May 10, 2024
Virtual event
| 8:30 a.m. Opening remarks – 5 minutes | |
|---|---|
| Presentations by faculty 10 minute presentation/ 5 minute Q&A |
|
| 8:35 a.m. | Dr. Alon Altman Postoperative venous thromboembolism in patients undergoing minimally invasive gynecologic oncology surgery |
| 8:50 a.m. | Dr. M. Nachtigal Interpretation of ovarian cancer risk and consideration of risk-reducing salpingo-oophorectomy in Hereditary Breast and Ovarian Cancer and Lynch Syndrome patients |
| 9:05 a.m. | Dr. A. Berard Molecular changes in the vaginal mucosal microenvironment of women after sexual intercourse |
| 9:20 a.m. | Dr. H. Pymar The CART Access Project: Advancing access to abortion for under-served populations through tools for healthcare professionals and people seeking care |
| 9:35 a.m. | Dr. C. Pylypjuk The FetUS is key! |
| 9:50 a.m. | Morning break |
| Project proposal — trainees 5 minute presentation/ 10 minute Q&A |
|
|---|---|
| 10:05 a.m. | Dr. Neil Reed External validation of the Modified Early Obstetric Warning System to predict maternal outcome in COVID-19 pneumonia |
| 10:20 a.m. | Dr. Honzer Chen Reproductive Factors Influenced by Composition of Vaginal Microbiome |
| 10:35 a.m. | Dr. Harley Bray The impact of COVID-19 and social distancing on sexual health education and adolescent pregnancy |
| 10:50 a.m. | Dr. Harley Bray The impact of social and gender norms on menstruation knowledge, attitudes, and practices in Sub-Saharan Africa |
| 11:05 a.m. | Dr. Anmol Mann The impact of abnormal fetal Dopplers on perinatal outcomes for infants born preterm at <32 weeks gestation: A retrospective cohort study |
| Completed work presentations — trainees 10 minute presentation/ 5 minute Q&A |
|
|---|---|
| 11:20 a.m. | Kaitlyn Quinlan "SKP" the CIN in High Grade Serous Ovarian Cancer |
| 11:35 a.m. | Sara Crooks GAELs: a potential new treatment option for high-grade serous ovarian cancer patients |
| 11:50 a.m. | Lunch break |
| Completed work presentations — trainees 10 minute presentation/ 5 minute Q&A |
|
|---|---|
| 1:00 p.m. | Dr. Catharine Zuzek-Friesen Factors associated with higher hospital resource utilization during term birth |
| 1:15 p.m. | Chelsea Day Trends in prenatal diagnosis of congenital gastrointestinal (GI) anomalies: a cohort study |
| 1:30 p.m. | Diana Prince Relationship between prenatal care during the pandemic and rates of stillbirth |
| 1:45 p.m. | Guneet Uppal Investigating perinatal factors associated with stillbirths during the COVID-19 pandemic: a cohort study |
| 2:00 p.m. | Emelissa Valcourt How common is an abnormal cerebroplacental ratio (CPR) at term? |
| 2:15 p.m. | * Dr. Catherine Lu Management of the placenta accreta spectrum disorders: a tertiary centre’s experience over 10 years |
| 2:30 p.m. | * Dr. Hailey Benoit Establishing barriers to improving perioperative feedback and increasing completion rates of assessment forms in an Obstetrics and Gynecology residency training program |
| 2:45 p.m. | * Dr. Marie Jones Manitoba's Distribution of Obstetrical Care and Patient Relocation for Delivery |
| * Eligible for Dr. Michael Helewa Research Day Award | |
| 3:00 p.m. | Afternoon break |
| Keynote speaker 45 minutes/ 15 minute Q&A |
|
|---|---|
| 3:15 p.m. | Dr. Chelsea Ruth My Clinician Researcher journey – Quite the adventure! |
| 4:15 p.m. | Closing remarks — 10 minutes |
Community and outreach
Manitoba Obstetric Outreach Program
The Manitoba Obstetric Outreach Program was established to address the discordance between Manitoba’s Aboriginal perinatal outcomes and those of the general Canadian population.
With honours, the program was the recipient of the 2006 Award for Excellence at St. Boniface General Hospital. This is in recognition of the program's support and promotion of the health of pregnant women in rural Manitoba
Contact us
Kemorine Platt
Coordinator, Manitoba Obstetric Outreach Program
Woman & Child Program
Hôpital St-Boniface Hospital
N5042 – 431, av. Taché Ave.
Winnipeg, Manitoba R2H 2A6
Phone: 204-237-2547
Fax: 204-233-1751
kplatt@sbgh.mb.ca
Goals and objectives
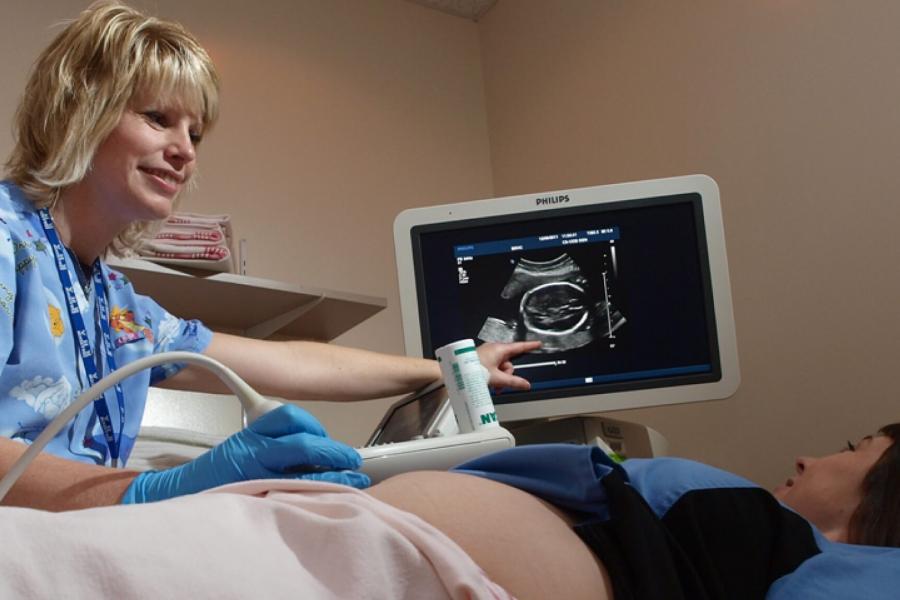
Provide point of care obstetric ultrasound and fetal assessments to rural Manitoba
Provide point of care obstetric ultrasound and fetal assessments to rural Manitoba
The program serves four reserves (Island Lake-Red Sucker Lake, Wasagamach, St. Therese Point, Garden Hill, Norway House, Little Grand Rapids & Pauingassi, and Berens River), which are reached by air several times throughout the year.
The portable ultrasound technology that we provide on site allows fetal Doppler examinations when needed.
The obstetric implications of accurate pregnancy “dating” are significant.
Approximately 40% of program assessments are to assist accurate estimation of gestation when patient menstrual dates are uncertain or unknown.
Provide point of care obstetric consultation
The program offers obstetric perinatal consultation when needed via the medical director and on site by an obstetrician during air visits.
It is not simply a technical (ultrasound) reporting service. All assessments provide a written report to the referring physician or midwife.
More complicated situations result in a letter or, if needed, a telephone interpretation and discussion between the medical director and provider of care.
Assistance arranging transfer to and consultation in Winnipeg’s tertiary care obstetric facilities is provided when necessary.
Improve perinatal morbidity and mortality
Although areas with higher perinatal mortality rates were originally selected for program visits, such rates for those sites decreased rapidly and now are comparable to the provincial rate.
Provided that patients with pregnancy complications are referred to the Program, their odds of perinatal deaths are similar to the provincial average.
Improve pregnancy outcomes of Indigenous patients
The program was designed to focus in particular on Indigenous patients, whose pregnancy outcomes remain worse than those of the rest of Canada’s population.
Although Manitoba’s population is approximately 15% identifiably Aboriginal, roughly three quarters of program assessments are Aboriginal patients, with some variance between sites.
Minimize family and social disruption
These consultations reduce disruption of families, avoiding unnecessary transfers and assessments in Winnipeg for most patients.
However, program services also improve identification of patients who need urban tertiary care.
When follow up examination of patients is required it may be arranged on subsequent site visits, or when needed in the Winnipeg Fetal Assessment Units.
Only ~5% of patients are recommended for transfer to Winnipeg and the average ultrasound number per patient is 1.5, well below the provincial average.
As well, significant economic and social effects for the isolated Island Lake population have been demonstrated by the J.A. Hildes Northern Medical Unit.
Improve effective use of obstetric diagnostic services
Data collected by this unique model have been informative and have implications for effective rural maternity care planning.
Issues may include (but are not limited to):
- Early pregnancy dating
- Placental localization given bleeding
- Early identification of multiple gestation
- Planning site of delivery in advance
- Arranging tertiary level consultation when problems are identified or confirmed
- Fetal anatomy review (19-22 week window)
Faculty and staff
Our award-winning faculty
Our team
Our faculty and staff are committed to supporting learners, colleagues and the community. Contact us to learn more about our department and what we have to offer.
You may also be looking for...
News and stories
View more news and stories-
Apr
24adMare Academy BioInnovation Scientist Program: Industry Essentials
12:00 AM
-
Apr
24Praxis Series: Identifying and Addressing Inadequacies in Musculoskeletal Medical Education Across Canada
11:00 AM
Online Zoom Session -

Apr
24Community Engagement of Sexual and Gender Minorities
12:00 PM
Online
Contact us
Obstetrics, Gynecology and Reproductive Sciences
260 Brodie Centre - 727 McDermot Avenue
University of Manitoba, Bannatyne Campus
Winnipeg, MB R3E 3P5 Canada